SARS-COV-2, COVID-19, and the brain
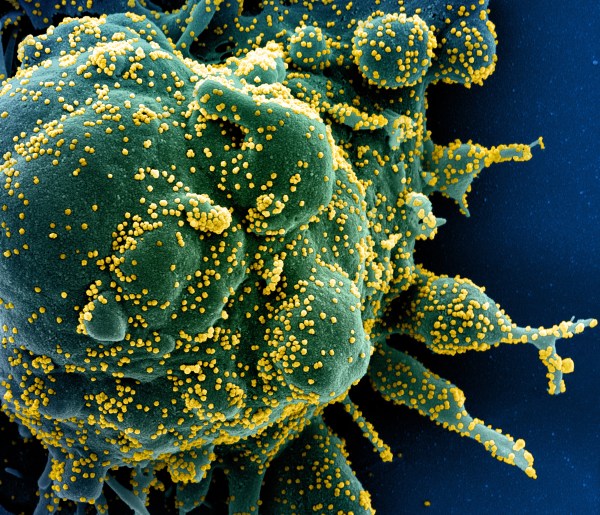
The novel coronavirus can invade the brain and has shown up in the cerebrospinal fluid. There is now evidence that many patients who appear to have recovered from COVID-19 have subtle alterations in their brains, which may be due to low-grade viral invasion.
The significance of these findings is primarily in that it may explain why so many people who think they have recovered are still having problems with fatigue/lassitude (that is, not on exertion like from a weak heart), loss of memory, and even depression.
Previous MRI (magnetic resonance imaging) studies have focussed on patients with severe, acute illness who have signs of stroke or brain hemorrhage, or else various neurological disorders suggesting encephalitis (or other major problems.)
Scroll down to the last study excerpted in this post for the “subtle brain alterations”– be prepared for “diffusion tensor imaging”– which will be explained in this article.
This study, which was just published in Lancet yesterday, August 3, uses diffusion tensor imaging to show that there are alterations in several brain regions which don’t rise to the level of dead tissue or blood clots, but still might mean that there is significant damage. I saved it for last because the other studies show the more serious things that can happen in severe illness.
Strokes and hemorrhages
Here is an MRI examination of 37 patients with severe COVID-19: half of them had hemorrhage (“stroke”). From the Results:
Thirty men (81%) and 7 women (19%) met inclusion criteria, with a mean age of 61+/- 12 years (range: 8-78). The most common neurologic manifestations were alteration of consciousness (27/37, 73%), pathological wakefulness when the sedation was stopped (15/37, 41%), confusion (12/37, 32%), and agitation (7/37, 19%). The most frequent MRI findings were: signal abnormalities located in the medial temporal lobe in 16/37 (43%, 95% CI 27-59%) patients, non-confluent multifocal white matter hyperintense lesions on FLAIR and diffusion sequences, with variable enhancement, with associated hemorrhagic lesions in 11/37 patients (30%, 95% CI 15-45%), and extensive and isolated white matter microhemorrhages in 9/37 patients (24%, 95% CI 10-38%). A majority of patients (20/37, 54%) had intracerebral hemorrhagic lesions with a more severe clinical presentation: higher admission rate in intensive care units, 20/20 patients, 100% versus 12/17 patients, 71%, p=0.01; development of the acute respiratory distress syndrome in 20/20 patients, 100% versus 11/17 patients, 65%, p=0.005. Only one patient was positive for SARS-CoV-2 RNA in the cerebrospinal fluid.
https://doi.org/10.1148/radiol.2020202222
Another study of 27 patients with neurological problems; Results:
Brain MRI was performed in 27/50 (54%) patients with neurologic symptoms (Fig 1). The median age of patients with MRI was 63 years (range 34-87 years, 21 males) (Table). 12/27 (44%, 95%CI 25-65%) patients who had MRI had acute findings. In 10/27 (37%) patients, cortical FLAIR signal abnormality (Fig 2; Appendix E1, Figs E1-E4) was present. Accompanying subcortical and deep white matter signal abnormality on FLAIR images were each present in 3 patients. Abnormalities involved the frontal lobe in 4, parietal lobe in 3, occipital lobe in 4, temporal lobe in 1, insular cortex in 3 and cingulate gyrus in 3 patients.
Cerobrospinal fluid (CSF) was obtained in 5 out of 10 patients with cortical signal abnormalities. Total protein was elevated (mean 79.9 mg/dL, range 59.9 – 109.7 mg/dL) in 4 of these patients. The cell count, glucose levels, IgG index, albumin were within normal limits, and RT-PCR for HSV DNA and SARS-CoV-2 were negative in all 5 specimens. Oligoclonal bands were checked in 3 specimens and were negative.
Other acute intracranial findings in the absence of cortical signal abnormality included 1 patient with acute transverse sinus thrombosis and 1 patient with acute infarction in right middle cerebral artery territory.
In 15/27 cases (56%), MR did not reveal any COVID-19 related or acute intracranial findings. CSF was obtained in two of these cases which showed elevated CSF protein (mean 98 mg/dL) despite negative MRI. A full description of MRI findings is in the supplement at the end of this article (Appendix E1).
https://pubs.rsna.org/doi/10.1148/radiol.2020201697
From an autopsy study, the Results:
Among the 62 patients who died from COVID-19 from 31/03/2020 to 24/04/2020 at our institution, 19 decedents fulfilled the inclusion criteria. Parenchymal brain abnormalities were observed in 4 decedents: subcortical micro- and macro-bleeds (2 decedents), cortico-subcortical edematous changes evocative of posterior reversible encephalopathy syndrome (PRES, one decedent), and nonspecific deep white matter changes (one decedent). Asymmetric olfactory bulbs were found in 4 other decedents without downstream olfactory tract abnormalities. No brainstem MRI signal abnormality was observed.
https://n.neurology.org/content/early/2020/06/16/WNL.0000000000010116
Loss of smell (anosmia)
A single 25 y/o patient with anosmia had this:
A 25-year-old female radiographer with no significant medical history who had been working in a COVID-19 ward presented with a mild dry cough that lasted for 1 day, followed by persistent severe anosmia and dysgeusia. She did not have a fever. She had no trauma, seizure, or hypoglycemic event. Three days later, nasal fibroscopic evaluation results were unremarkable, and noncontrast chest and maxillofacial computed tomography results were negative. On the same day, a brain MRI was also performed. On 3-dimensional and 2-dimensional fluid-attenuated inversion recovery images, a cortical hyperintensity was evident in the right gyrus rectus (Figure 1) and a subtle hyperintensity was present in the olfactory bulbs (Figure 1). Because many patients in Italy are experiencing anosmia (https://academic.oup.com/cid/article/71/15/889/5811989) and the cortical signal alteration was suggestive of viral infection, a swab test was performed and reverse transcription–polymerase chain reaction analysis yielded positive results for SARS-CoV-2. During a follow-up MRI performed 28 days later, the signal alteration in the cortex completely disappeared and the olfactory bulbs were thinner and slightly less hyperintense (Figure 24). The patient recovered from anosmia. No brain abnormalities were seen in 2 other patients with COVID-19 presenting anosmia who underwent brain MRI 12 and 25 days from symptom onset.
https://jamanetwork.com/journals/jamaneurology/fullarticle/2766765
But then a larger study showed “nonspecific white matter angiopathy”:
Two hundred forty-two patients with COVID-19 underwent CT or MRI of the brain within 2 weeks after the positive result of viral testing (mean age, 68.7 ± 16.5 years; 150 men/92 women [62.0%/38.0%]). The 3 most common indications for imaging were altered mental status (42.1%), syncope/fall (32.6%), and focal neurologic deficit (12.4%). The most common imaging findings were nonspecific white matter microangiopathy (134/55.4%), chronic infarct (47/19.4%), acute or subacute ischemic infarct (13/5.4%), and acute hemorrhage (11/4.5%). No patients imaged for altered mental status demonstrated acute ischemic infarct or acute hemorrhage. White matter microangiopathy was associated with higher 2-week mortality (P < .001). Our data suggest that in the absence of a focal neurologic deficit, brain imaging in patients with early COVID-19 with altered mental status may not be revealing.
http://www.ajnr.org/content/41/7/1179
Diffusion Tensor Imaging
Finally, a study using diffusion tensor imaging in MRI scans showed numerous subtle alterations during the recovery phase. This from the Findings and Interpretation:
In this follow-up stage, neurological symptoms were presented in 55% COVID-19 patients. COVID-19 patients had statistically significantly higher bilateral gray matter volumes (GMV) in olfactory cortices, hippocampi, insulas, left Rolandic operculum, left Heschl’s gyrus and right cingulate gyrus and a general decline of MD [mean diffusivity], AD [axial diffusivity], RD [radial diffusivity] accompanied with an increase of FA [fractional anisotropy] in white matter, especially AD in the right CR [corona radiata], EC [external capsule] and SFF [superior fronto-occipital fasciculus], and MD in SFF compared with non-COVID-19 volunteers (corrected p value <0.05). Global GMV [gray matter volume], GMVs in left Rolandic operculum, right cingulate, bilateral hippocampi, left Heschl’s gyrus, and Global MD of WM [white matter] were found to correlate with memory loss (p value <0.05). GMVs in the right cingulate gyrus and left hippocampus were related to smell loss (p value <0.05). MD-GM score, global GMV, and GMV in right cingulate gyrus were correlated with LDH [lactate dehydrogenase] level (p value <0.05).
Study findings revealed possible disruption to micro-structural and functional brain integrity in the recovery stages of COVID-19, suggesting the long-term consequences of SARS-CoV-2.
https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(20)30228-5/fulltext