New strains of SARS-COV-2, from South Africa, Britain, Brazil, and elsewhere: more contagious and possibly more lethal. Sequencing is essential.
New strains of SARS-COV-2 have appeared in the United States recently. This is inevitable and foreseeable. One strain, first seen in Britain, has been tested and found to be more contagious than the original strains. Another strain, both more contagious and possibly more lethal, has been found in South Africa and may soon appear in the US. A third originates from Brazil and was found here (in Minnesota) in a traveler from there.
The Centers for Disease Control (CDC) has published a paper on January 15, 2021 outlining current knowledge about the new strains. At the time this was published, the Brazilian variant had not been seen in the US (further discussion about surveillance below).
From the CDC paper:
In the United Kingdom (UK), a new variant called B.1.1.7 has emerged with an unusually large number of mutations. This variant spreads more easily and quickly than other variants. Currently, there is no evidence that it causes more severe illness or increased risk of death. This variant was first detected in September 2020 and is now highly prevalent in London and southeast England. It has since been detected in numerous countries around the world, including the United States and Canada.
In South Africa, another variant called 1.351 has emerged independently of the variant detected in the UK. This variant, originally detected in early October, shares some mutations with the variant detected in the UK. There have been cases caused by this variant outside of South Africa, but it has not been detected in the US.
In Brazil, a variant called P.1 emerged and was identified in four travelers from Brazil, who were tested during routine screening at Haneda airport outside Tokyo, Japan. This variant contains a set of additional mutations that may affect its ability to be recognized by antibodies. This variant has not been detected in the US.
https://www.cdc.gov/coronavirus/2019-ncov/transmission/variant.html
Note that these variants are found by sequencing viruses isolated from human samples taken to detect infections. Currently, in the US, surveillance is weak: less than 0.3% of isolates are sequenced. In Britain, by contrast, nearly 10% of isolates have been sequenced. The detection of SARS-COV-2 in patients with COVID-19 by RT-PCR (reverse transcriptase-polymerase chain reaction) depends on certain signatures found in the SARS-COV-2 virus proteins; false-negative results in one of the three separate analyses can result from mutations in the virus RNA that cause changes in the spike protein, in particular.
Once the virus has been detected by RT-PCR, if there is a sufficient number of virions, the virus’ genetic code can be sequenced to find mutations. This process is essential for surveillance for several reasons. The first is that every isolate from a single patient is likely to contain at least one mutation from the isolate from other patients. This allows scientists to determine the likely source of the individual patient’s infection.
Another reason is that groups of mutations that have significant effects on the virus’ ability to spread (its contagiousness) or its lethality (the severity of the resulting infection) can be detected and adjusted for.
The vaccine in use in the US today, whether from Moderna or Pfizer, is based on MRNA (messenger ribonucleic acid) which is ingested by the patient’s individual cells and used to transcribe into proteins (just like the body’s normal mRNA, constantly produced in the process of cell metabolism). The mRNA codes for the spike protein, which, when synthesized in the body, provokes an immune reaction that produces antibodies and primes immune cells to recognize and attack the virus.
Mutations that change the spike protein can and do affect the ability of the vaccine to produce effective antibodies. If a virus were to have sufficiently different spike proteins than the protein produced by the vaccine, it would become ineffective. Indeed, one mutation recently discovered reduces the effectiveness of the vaccine six-fold. Luckily, the immune reaction is so intense that the body produces 800 times as many antibodies (and immune cells) as are needed to fight off the virus.
Therefore, the current vaccine is expected to be effective against the new strains of virus, at least for now. In the near future, it will be necessary to produce a different vaccine to account for the mutations yet to arise. In fact, Moderna has already begun developing a new version of its vaccine. (More information about the new variants can be found in the same NYT article.)
Again, luckily, the process of producing a new vaccine is quick and easy; one scientist estimated that it would take about six weeks to create an entirely new mRNA vaccine from scratch. If the Food and Drug Administration is sufficiently receptive to rapid changes in this vaccine (which makes perfect sense because the differences would be trivial and previous clinical trials have clearly established the vaccine’s safety), the new vaccine could be available within a couple of months whenever it is thought necessary to make a change.
In this respect, however, one thing needs to be changed in the US: our surveillance capabilities. We must sequence several times as many virus isolates as we do now. We should aim to sequence 10% of the viruses obtained from RT-PCR tests, just as they do in Britain. This depends on a government subsidy to labs that do this sequencing and collation of the results into databases. The information will inform us of new variants and at the same time make contact tracing much easier by enabling the tracing of mutations from one host (infected person) to the next.
An organization called NextStrain has been collating the sequences of SARS-COV-2 genomes as they are reported, although they have been hampered by poor support from the US federal government. A very out-of-date situation report is available here (from August).
At the same time, prevention of transmission by mask-wearing, hand-washing, and isolation still works, even if the virus is more contagious than before. So it is essential that we continue these preventive measures at least until herd immunity is attained in the US.
Estimates of when herd immunity will be reached in this country have generally been in the range of June to October of this year; other countries may not achieve protected status until 2022 at the earliest. Positive test results have so far been found in about 7% of the US, while estimates of actual infection rates range up to 20% or more. Some counties (eg, in Arizona and Texas) are reporting case rates of 0.1-0.2% per day (see New York Times interactive page for details.)
I have blogged about this before, but it bears repeating: one aspect of our federal government’s response to this pandemic must be provision of sufficient funds and administrative efforts to perform sequencing and gathering the data about virus signatures. Plenty of labs and equipment are available; what is needed is money and administrative time. There are many other things that must be done, and they all require money, lots of it, from the federal government, along with organization and direction from the top. Anthony Fauci, MD is an ideal person to direct this effort, and he has been placed at the head of the US effort. By the way, he received the Presidential Medal of Freedom back in 2008, when it meant something.
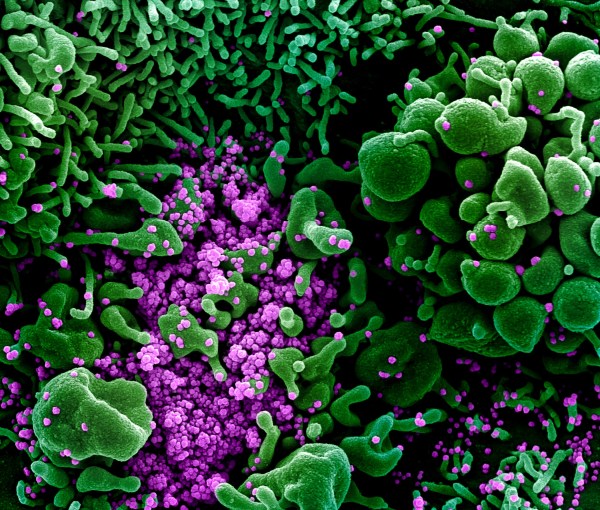
(photo: sars-cov-2 budding from apoptotic cells–electron microscopy by NIAID)